Symptoms
Early detection of ovarian cancer is challenging because symptoms can be mild and vague and could apply to a variety of conditions, such as irritable bowel syndrome or ovarian cysts.
However, the most typical ovarian cancer symptoms, or changes that someone may feel, include:
-
- Swollen or bloated abdomen
- Persistent pain in the abdomen or pelvis
- Difficulty eating, constantly feeling full
- Increased urination
Other symptoms such as constipation or diarrhea, fatigue, back pain, and spotting between periods are also reported by people with ovarian cancer.
Since these symptoms are also seen with many other common conditions, and a person may only become aware of the symptoms after the tumor has grown or has started to spread, it is common for ovarian cancer to be diagnosed in later stages.
There are no effective screening tests for ovarian cancer. Therefore, if you have symptoms that are new and last for more than a few weeks, you should report them to a healthcare professional as soon as possible.
Ovarian cancers, fallopian tube cancers, and primary peritoneal cancers are similar, and they are treated the same way. In these diseases, cancer cells form in the epithelial tissue covering the ovaries, in the lining of the fallopian tubes, or in the peritoneal membrane that lines the abdomen and organs in the abdomen. On our website, when the term “ovarian cancer” is used, it includes fallopian tube cancers and primary peritoneal cancers.
Stages
One of the most important steps in treating ovarian cancer is staging the disease. In other words, has it spread, and, if so, how far? Knowing the stage of cancer guides the treatment plan, helps someone find clinical trial options, and gives information about what an individual can expect going forward.
Staging is generally done during surgery, placing the cancer in one of four categories:
Stage 1
The cancer is limited to one or both ovaries or to the fallopian tubes. 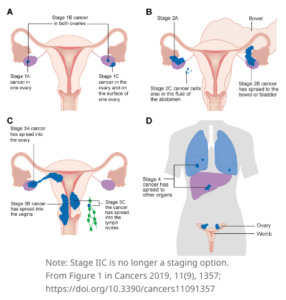
- 1A- cancer is in one ovary or one fallopian tube
- 1B- cancer is in both ovaries or both fallopian tubes
- 1C- cancer is in and on the surface of one or both ovaries
Stage 2
The cancer has spread to other areas of the pelvis, uterus, bladder, colon, or rectum.
- 2A- cancer has grown into the uterus and/or fallopian tubes
- 2B- cancer is found in other organs in the pelvis like the bladder, colon, or rectum
Stage 3
The cancer has spread to the abdomen and may also be in the lymph nodes. Primary peritoneal cancers are stage 3.
- 3A1- cancer has spread to the lymph nodes in the back of the abdomen
- 3A2- cancer has spread to the tissue lining the abdomen, but is so small it can only be seen under a microscope
- 3B- cancer can be seen on the lining of the abdomen but is 2 centimeters or smaller
- 3C- cancer can be seen on the lining of the abdomen and is larger than 2 centimeters. Cancer may also be found on the outer layer of the liver or spleen.
Stage 4
The cancer has spread to organs outside the abdomen.
- 4A- cancer is found in the fluid surrounding the lungs (called a malignant pleural effusion)
- 4B- cancer is found inside the liver or spleen, in distant lymph nodes, or has spread to other organs outside of the abdomen
Types of Ovarian Cancer
The treatment people receive for ovarian cancer depends on their specific type and grade of cancer (histology).
The type and grade of ovarian cancer are determined by sending a part of the tumor tissue to a pathologist who looks at the tissue under a microscope. Tissue can be taken during surgery or a biopsy. A biopsy is a procedure in which a small amount of tissue is taken from the tumor or the fluid surrounding the tumor.
The grade of cancer is different from the stage of cancer. The grade of cancer has to do with how fast the cancer cells grow (high-grade grows faster than low-grade), whereas the stage of cancer has to do with the size and location of the cancer.
There are three major ovarian cancer types based on where the tumor develops:
- Epithelial tumors account for 90 percent of ovarian cancers and start from cells on the outside of the ovaries (the epithelium), the fallopian tubes, or the peritoneal membrane surrounding organs in the abdomen or pelvis. There are multiple types (histologies) of epithelial ovarian cancer. The most common are:
-
- High-grade serous
- Clear cell
- Mucinous
- Endometrioid
- Carcinosarcoma
- Low-grade serous
- Germ cell tumors originate inside the ovaries in the cells that create the eggs. These tumors are rare and generally affect younger women.
- Stromal tumors are also rare and originate in the connective tissue surrounding the ovaries.
Genetic Testing for Inherited Mutations
Every cell of the body has two copies of every gene – one copy that is inherited from an individual’s mother and one copy from their father. Inherited genes may have mutations (changes) that can increase the risk of developing cancer.
Genetic testing looks for inherited changes in specific genes that are known to be associated with an increased risk of getting cancer. Any person with an ovarian cancer diagnosis should have genetic testing done to determine if they have inherited a changed version of one or more of such genes from one of their parents. Inherited changes would be present in every cell in the body, so genetic testing is done on a sample of saliva or blood.
Mutated Genes Associated with Ovarian, Fallopian Tube, or Primary Peritoneal Cancer
Sometimes, ovarian cancer has a hereditary element — an individual may have someone in their family who has also had breast or ovarian cancer. The most commonly mutated genes we know to be associated with an increased risk of developing ovarian cancer are BRCA1 and BRCA2. There are other genes e.g. PALB2, RAD51C/D that, when changed, are also known to be associated with an increased risk of developing ovarian cancer. Often, when genetic testing is ordered, testing will look for changes in these and other specific genes. Therefore, this testing is also referred to as panel testing. Another term used to describe genetic testing is germline testing.
The Role of Genetic Counselors
Genetic testing has the opportunity to reveal inheritable conditions that can potentially affect other family members and be passed down to children. Due to the complexity of emotions that often accompany this reality, it is recommended that an individual seek genetic counseling before and after testing. Genetic counselors are experts who can help someone understand their genetic testing results, clarify risks for additional cancers, and support someone in the process of sharing their results with relatives and children. The healthcare team can make a referral to a genetic counselor or a genetic counselor can be found through the National Society of Genetic Counselors.
Tumor Biomarker Testing
Genetic testing looks for genetic changes that are present in every cell in the body. However, sometimes in cancer cells, abnormal changes occur only in the tumor.
Tumor biomarker testing looks for changes in the cancer cells. Tumor biomarker testing may be done on a sample of the cancer obtained during surgery or biopsy. It may also be done on a cancerous fluid sample or a blood sample (liquid biopsy). Tumor biomarker testing is also sometimes called molecular profiling, genomic testing, somatic testing, tumor profiling, or tumor testing.
What is a Biomarker?
A biomarker is a substance in the body that can be measured and can give information about someone’s health. In cancer, biomarkers are abnormal changes that cause cancer to survive and grow. Tumor biomarker testing is a way for doctors to gather as much information as possible about an individual’s unique type of cancer. This information is used to offer the most appropriate treatment options.
Common Tumor Biomarkers for Ovarian, Fallopian Tube, or Primary Peritoneal Cancers
Biomarkers have different names which are often 3 or 4-letter abbreviations that may also contain numbers. Depending on what tumor biomarker tests are performed after an ovarian cancer diagnosis, biomarker test results could include:
- HRD (homologous recombination deficiency)/LOH (loss of heterozygosity)
- MMR (mismatch repair)
- MSI (micro-satellite instability)
- TMB (tumor mutational burden)
- Folate Receptor alpha (FRalpha, FOLR1)
- HER2
- Genes known to be associated with cancer (BRCA1/2, TP53, BRAF, NTRK, RET, etc.)
How is a Tumor Biomarker Test Done?
Doctors use a tumor sample that has already been removed and stored, or they schedule a biopsy to collect fresh tumor tissue that can be sent to a laboratory. Blood samples may also be collected. Next, the laboratory performs tests to look for specific biomarkers in the sample(s). A tumor biomarker test report is sent to the doctor and the patient when the results are ready.
Tumor Biomarker Testing and Targeted Therapies
Tumor biomarker testing may provide important information to help guide treatment decisions. In some cases, there is an approved drug for patients with specific biomarkers found in their tumor. In other cases, the presence of specific changes in the tumor are required for people to enroll in some clinical trials that are testing drugs that are predicted to work for them. As research progresses and new targeted therapies are developed and approved, additional biomarker testing may be ordered to inform treatment options.
Clearity Can Help
Clearity can help people understand the results of their tumor biomarker testing. Clearity’s team includes experts in ovarian cancer molecular and cellular biology. They can help you understand your testing results, the unique nature of your cancer, as well as potential treatments and clinical trial options available to you. Learn more.

